Missing teeth change more than the look of your smile—they influence how you chew, how your jaw ages, and how you feel about yourself. Tooth loss is common across the U.S., and modern implant dentistry offers a predictable way to restore both function and appearance. Instead of relying on removable solutions alone, implants re-establish a foundation in the jaw that supports lifelike crowns, bridges, or full-arch restorations.
Because implants fuse with the bone, they provide a level of stability and sensation that removable options can’t match. The result is often a return to normal eating, clearer speech, and much less worry about shifting or slipping prosthetics. For many patients, that stability translates into confidence in daily life—eating in public, laughing with friends, and speaking without hesitation.
At Complete Dental Care of Fishers, we focus on clinical planning and clear communication so patients understand their options and the expected outcomes. Whether you’re replacing a single tooth or rebuilding an entire arch, a thoughtful implant plan centers on long-term health, predictable results, and a natural-looking final smile.

Dental implants are small, biocompatible posts that act like tooth roots. Once an implant integrates with the surrounding bone, it becomes a secure anchor for a crown, bridge, or denture. That root-level support gives implant restorations a natural bite force and prevents the movement often seen with traditional removable dentures.
Unlike a conventional bridge that depends on your adjacent teeth for support, an implant restoration can stand on its own. This avoids the need to permanently alter healthy neighboring teeth and preserves more of your natural structure. The result is a restoration that functions like a natural tooth while also protecting the long-term health of the surrounding dentition.
Modern restorative materials and careful shade-matching techniques help implant crowns blend seamlessly with natural teeth. When properly designed, implant-supported restorations are virtually indistinguishable from real teeth in appearance and feel.
A dental implant system typically includes three parts: the implant (a titanium or similar metal post), an abutment that connects the post to the visible restoration, and the prosthetic crown, bridge, or denture. Each component plays a role in stability, hygiene, and how the restoration looks and functions in the mouth.
The implant itself is designed to encourage bone to grow around it—a process called osseointegration. This biological bonding is what gives implants their long-term stability and supports normal chewing forces. The abutment and final restoration are shaped and colored to match your bite and smile, creating a functional and aesthetic result.
Planning is essential: diagnostics such as clinical exams and 3D imaging help determine implant size, position, and whether preparatory treatments like bone grafting are necessary. A clear plan reduces surprises and helps deliver predictable outcomes tailored to each patient.
Implants are favored because they address the common frustrations people experience with missing teeth: limited diet, shifting restorations, and gradual bone loss. By replacing the root as well as the tooth, implants preserve jawbone volume and support facial structure—benefits that go beyond aesthetics.
When well planned and maintained, an implant restoration can last for many years. Since implants don’t develop cavities, the maintenance focus is on keeping surrounding tissues healthy with good home care and regular professional checkups. That combination helps protect both the implant and your remaining natural teeth.
Because implants feel and function like natural teeth, patients frequently report improved comfort and confidence. Treatments can range from a single tooth replacement to implant-supported full-arch solutions, allowing a tailored approach depending on the clinical situation and the patient’s goals.
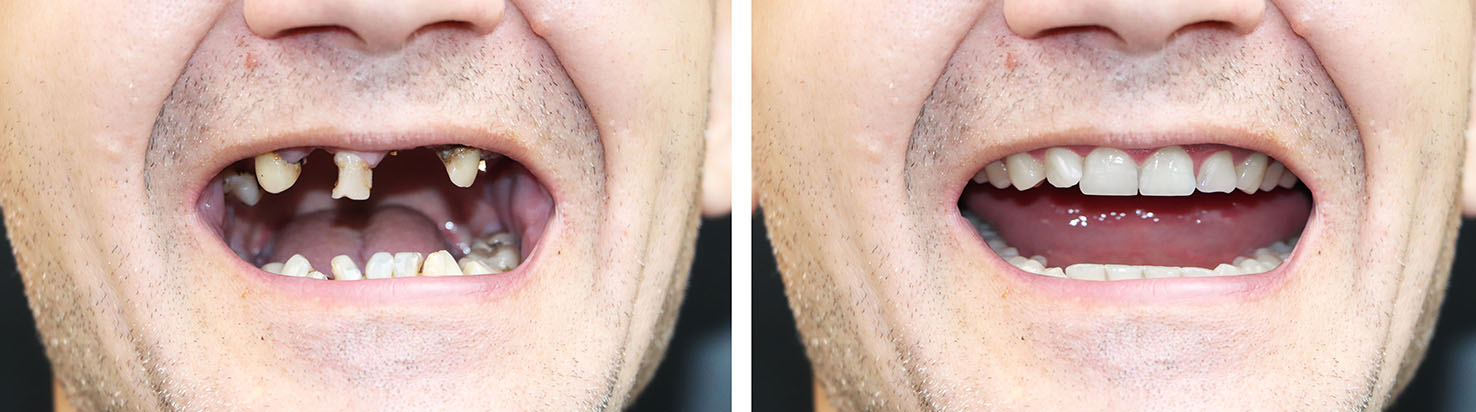
When only one tooth is missing, a single implant topped with a custom crown replaces both the look and the function of that tooth without altering neighboring teeth. This approach preserves healthy enamel and provides a long-lasting, easy-to-care-for solution that fits naturally into your smile.
For two or more adjacent missing teeth, implants can support a bridge without using natural teeth as anchors. Strategically placed implants carry the load for multiple replacement teeth while maintaining the health and position of surrounding teeth. This preserves bone and offers a stable chewing surface compared with a traditional tooth-supported bridge.
Patients who are missing most or all of their teeth may benefit from a full-arch implant restoration supported by multiple implants. These solutions recreate an entire dental arch that is fixed in place and behaves like natural teeth, offering improved function, comfort, and appearance without the need for daily removal.
When a removable prosthesis is preferred or required, attaching a denture to a few implants dramatically improves retention and stability. Implant-retained overdentures eliminate many common denture frustrations—slippage, sore spots, and adhesive dependence—while still allowing easier removal for cleaning if the patient desires.
Most adults who are in generally good health and have adequate bone are potential candidates for dental implants. Factors such as uncontrolled medical conditions or heavy tobacco use can complicate healing, but many situations can be managed or improved with targeted treatments and collaboration between dental and medical providers.
Bone volume and quality are important considerations. If bone has resorbed after tooth loss, bone grafting or sinus lift procedures can rebuild the foundation needed for stable implant placement. Advances in grafting materials and techniques make successful augmentation possible in many cases that were once considered unsuitable.
A thorough evaluation—including a clinical exam, dental imaging, and a review of your medical history—lets the care team design a plan that fits your oral health, lifestyle, and goals. Diagnostic tools like 3D imaging help the team choose the optimal implant position, size, and prosthetic approach for long-term success.
Implant treatment begins with a detailed plan that considers bite, esthetics, and existing dental health. Using diagnostic models and imaging, the team selects implant locations that support both function and a natural-looking smile. This planning reduces surprises and paves the way for efficient, predictable surgery.
Surgical placement of implants is typically performed on an outpatient basis and is considered a routine procedure in modern practice. Depending on the case, local anesthesia, oral sedation, or other comfort measures are used to keep patients relaxed. Most patients experience manageable discomfort that resolves within a few days.
Following placement, implants require time to integrate with the bone. In many situations, temporary teeth can be attached immediately to preserve appearance and function, while final restorations are fabricated and seated after full healing and integration.
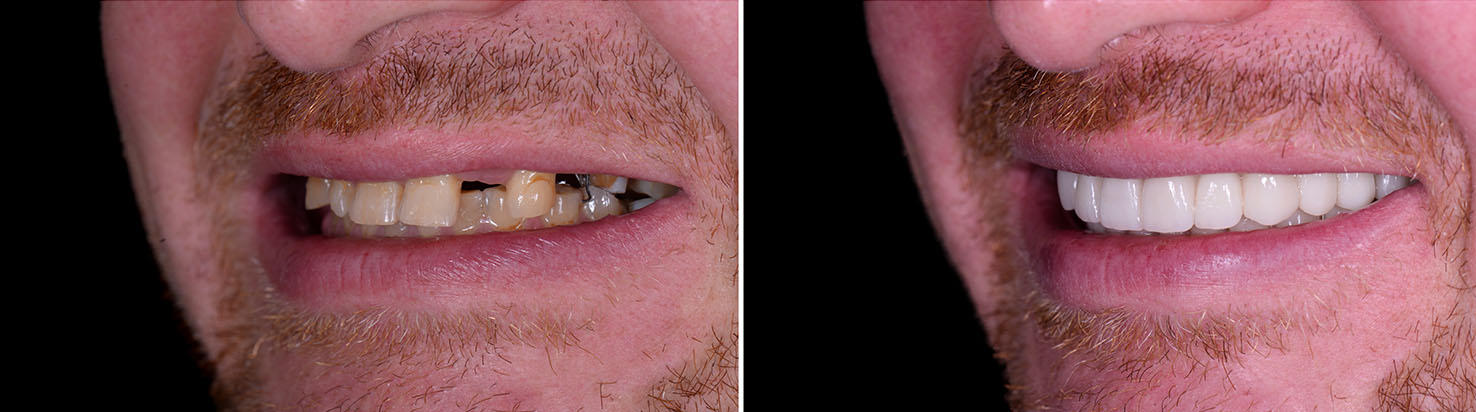
Bone grafting is a common and proven method to rebuild lost socket height or width where jawbone has diminished. Small grafts placed at the time of extraction or ahead of implant placement provide the structural support implants need to integrate and function long-term. Materials and techniques vary, but the objective is the same: create a stable foundation for the implant.
Healing time after grafting depends on the size and type of graft and the patient’s biology. Your clinician will explain timing and what to expect, and will coordinate grafting and implant placement in a way that optimizes outcomes and minimizes the number of surgical visits whenever clinically appropriate.
Replacing missing teeth with implants restores more than just teeth; it restores the ability to eat well, speak clearly, and smile with confidence. With careful planning, modern imaging, and attention to restorative detail, implant therapy can deliver outcomes that look natural, feel comfortable, and stand up to daily life.
If you’d like to learn whether implants are the right option for your smile, our team can explain the steps involved and help you understand what to expect. Contact us to speak with our office and start the conversation about rebuilding your smile.
Dental implants are biocompatible posts that replace a missing tooth root and serve as a stable anchor for a crown, bridge, or denture. Once placed in the jaw, the implant encourages bone to grow around its surface in a process called osseointegration, which creates a strong, long-term foundation. The visible restoration is attached to an abutment that connects the prosthetic to the integrated implant, restoring chewing function and appearance.
Because an implant replicates the root and supports a restoration from the base, implant-supported teeth resist movement and provide bite force similar to natural teeth. Modern implant systems use materials and precision components designed to promote tissue health and simplify hygiene. Careful planning and accurate placement are essential to ensure the implant functions and looks like a natural tooth for many years.
Implants preserve jawbone by replacing the missing root, which helps maintain facial contours and prevents the bone resorption commonly seen after tooth loss. They also restore chewing efficiency and speech because the implant-root support prevents the slipping or shifting that can occur with removable prosthetics. Unlike a traditional bridge, an implant restoration does not require the alteration of adjacent healthy teeth, preserving natural tooth structure.
Implants offer a predictable, long-term solution that simplifies daily care since the fixture itself cannot get a cavity and the focus is on maintaining healthy surrounding tissues. High-quality restorative materials and shade-matching techniques allow implant crowns and bridges to blend seamlessly with natural teeth. At Complete Dental Care of Fishers, implant planning emphasizes both function and esthetics to deliver stable, natural-looking results.
Most adults in generally good health with adequate jawbone are potential implant candidates, but candidacy depends on a comprehensive evaluation of oral and medical history. Factors such as smoking, uncontrolled diabetes, certain medications, or a history of radiation to the head and neck can affect healing and must be discussed with the dentist and medical providers as needed. Bone volume and quality are evaluated with clinical exams and imaging to determine whether grafting or other preparatory procedures are required.
Age alone is not a contraindication, and many patients who were once told they were not candidates can proceed after targeted treatments such as bone grafting or sinus augmentation. A personalized treatment plan based on 3D imaging, bite analysis, and restorative goals helps determine the best approach and timing for implant placement. Your clinician will review alternatives if implants are not the appropriate choice.
Treatment begins with a comprehensive consultation that includes a clinical exam, review of medical history, and diagnostic imaging to evaluate bone and plan implant position. The team develops a detailed restorative plan that considers esthetics, bite mechanics, and long-term maintenance, and discusses anesthesia or sedation options to ensure patient comfort during surgery. Surgical placement of the implant is performed in an outpatient setting and typically uses local anesthesia with additional comfort measures as needed.
After implant placement, a healing period allows osseointegration to occur; temporary restorations may be provided to preserve appearance and function during healing. Once integration is confirmed, an abutment is attached and the final crown, bridge, or denture is fabricated and seated to match adjacent teeth and bite relationships. Follow-up appointments monitor healing and confirm prosthetic fit and function.
Healing and osseointegration typically take several months, with many cases following a general timeline of about three to six months depending on the implant site and individual biology. Factors such as bone density, the need for grafting, the location in the mouth, and the patient’s overall health influence the rate of integration. During this period the implant becomes firmly anchored in the jaw, which is essential before loading it with a final restoration in many traditional protocols.
Some clinical situations allow for immediate provisionalization or earlier loading, but these approaches are case-dependent and require careful planning to avoid excessive forces during healing. Your clinician will outline an expected timeline tailored to your circumstances and will schedule follow-up visits and imaging to confirm successful integration before proceeding with the final prosthetic. Adhering to post-operative instructions and maintaining good oral hygiene supports timely healing.
Bone grafting is recommended when there is insufficient jawbone height or width to support an implant securely, which can occur after long-standing tooth loss, periodontal disease, or trauma. Grafting rebuilds the bone volume by placing bone graft material into the deficient site, creating a stable foundation for later implant placement. In the upper back jaw, a sinus lift may be required when the maxillary sinus floor is too close to the planned implant position.
Modern grafting materials and techniques make augmentation predictable, and grafts may be performed at the same time as implant placement in some cases or staged as a separate procedure when more extensive regeneration is needed. Healing time after grafting varies with the graft size and type, and your dentist will explain the sequence and expected healing intervals so implant placement can proceed safely and predictably. Close follow-up and imaging are used to assess graft maturation before proceeding.
Implant restorations range from single crowns for a missing tooth to implant-supported bridges, fixed full-arch restorations, and implant-retained overdentures for patients missing multiple teeth. A single implant with a crown replaces one tooth without altering adjacent teeth, while two or more implants can support a bridge to replace several adjacent teeth. Fixed full-arch solutions use multiple implants to permanently replace an entire dental arch and restore function similar to natural teeth.
Implant-retained overdentures attach to a smaller number of implants to dramatically improve denture stability while allowing removal for cleaning if desired. Prosthetic materials and attachment methods are selected to match patient needs for esthetics, hygiene, and durability. Your restorative team will recommend the option that best fits your oral condition, functional needs, and long-term goals.
Daily oral hygiene is essential for implant health and includes brushing with a soft-bristled brush, cleaning around the implant with interdental brushes or floss, and rinsing as recommended by your clinician. Professional maintenance visits are important to remove plaque and check the surrounding tissues, and these visits allow early detection of issues such as mucosal inflammation or mechanical wear. Unlike natural teeth, implants cannot develop cavities, but the surrounding gum and bone still require attention to prevent peri-implant disease.
Patients with risk factors such as a history of periodontal disease, smoking, or bruxism may need more frequent follow-up and specialized prevention strategies like antimicrobial rinses or occlusal guards. Consistent home care combined with periodic clinical examinations and X-rays helps protect the implant and adjacent teeth and supports predictable long-term function. Your dental team will provide a customized maintenance schedule based on your individual risk profile.
As with any surgical procedure, dental implant placement carries risks such as infection, bleeding, damage to adjacent teeth, and temporary or rarely permanent nerve or sinus complications depending on implant location. Early recognition and prompt management of complications such as infection or soft-tissue irritation typically lead to favorable outcomes, so adherence to post-operative instructions and scheduled follow-up is important. Implant failure can occur if integration does not take place or if peri-implant infection develops, but careful planning and maintenance reduce these risks.
Long-term complications are often related to poor hygiene, uncontrolled medical conditions, or excessive occlusal forces, and many of these issues can be mitigated through patient education and preventive care. Your dentist will review your medical history and oral condition to identify and address risk factors before treatment, and they will explain signs to watch for so you can seek timely care if needed. Clear communication and monitoring help ensure implant therapy proceeds safely.
Begin by scheduling a consultation so the team can perform a clinical exam, review your medical history, and take diagnostic images to evaluate bone and neighboring structures. During the visit you can discuss your restorative goals, comfort options for surgery, and any preparatory treatments such as grafting that may be necessary. The clinician will explain the treatment sequence and answer questions about healing, function, and expected outcomes.
After the evaluation, the practice will present a personalized plan that includes recommended procedures and a proposed timeline for placement and restoration. You will receive instructions for pre- and post-operative care and a schedule of follow-up appointments to monitor healing and prosthetic fit. The team coordinates imaging and lab work and will guide you through each step so you understand what to expect from consultation through completion.
Email: