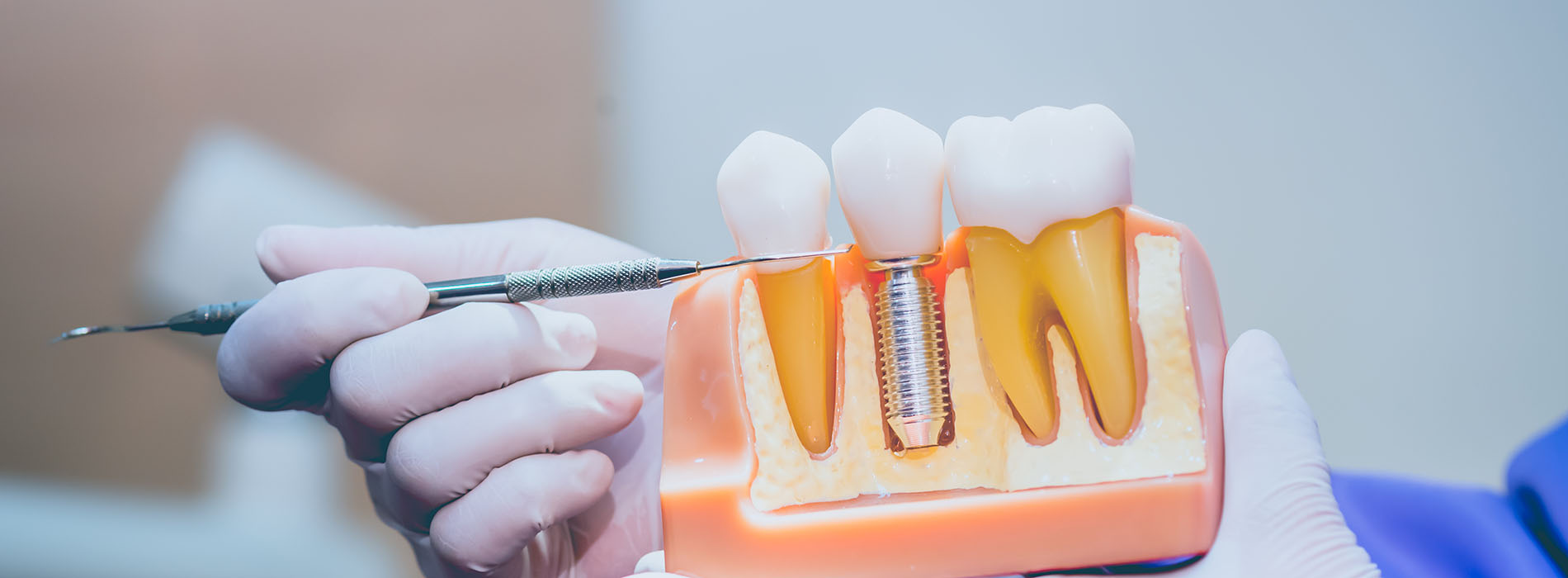
Replacing a missing tooth does more than restore a smile — it preserves function, supports surrounding teeth, and helps maintain jawbone health. Implant restorations are designed to reproduce the way a natural tooth looks, feels, and performs. By anchoring replacement teeth to titanium posts that fuse with the jaw, implant restorations provide stability that conventional removable options often cannot match, allowing patients to bite and speak with confidence.
Modern implant restorations are rooted in decades of clinical research and have become a predictable solution for a wide range of tooth-replacement needs. Their success stems from both the surgical integration of the implant and the craftsmanship of the final restoration. When planned and executed well, an implant-supported crown or bridge functions like a natural tooth and integrates seamlessly into your bite and smile.
For many patients, the long-term benefits include improved chewing efficiency and a natural appearance that supports self-confidence. The decision to pursue implant restorations is a collaboration between patient and clinician — one that balances oral health, aesthetic goals, and practical considerations to arrive at a personalized treatment plan.
Implant restoration begins after a dental implant has been placed and allowed time to integrate with the jawbone. Once osseointegration is complete, the restorative phase focuses on creating the visible replacement tooth or teeth. This phase typically starts with taking precise impressions or digital scans of the mouth, which capture the position of the implant and the relationship to adjacent teeth and soft tissues.
With these records, the restorative dentist designs a crown, bridge, or overdenture that matches the patient’s bite and smile line. Attention to detail is crucial: shade selection, tooth shape, and margin placement all influence how natural the finished restoration will look and feel. Many practices now use CAD/CAM technology to improve accuracy and reduce the number of visits, while still preserving the craftsmanship required for excellent esthetics.
The restoration is attached to an abutment that connects the prosthetic tooth to the implant post. Depending on the case, the abutment and the final restoration may be custom-made to optimize appearance and function. After placement, the dentist evaluates occlusion (bite), contours, and comfort, making minor adjustments if needed to ensure a smooth transition into everyday use.
Choosing the right materials is a key step in achieving a life-like implant restoration. Porcelain and zirconia are commonly used for crowns and bridges because they offer excellent strength and translucency that mimics natural enamel. Metal-based restorations may still be appropriate in some situations, but all-ceramic options are often preferred where esthetics are important.
Beyond material selection, how the restoration is shaped and finished affects how light reflects from the tooth and how it blends with adjacent teeth. A skilled restorative dentist considers subtle details such as the emergence profile (how the tooth appears to grow from the gum), surface texture, and color gradations. These elements help the restoration appear as though it has always been part of the smile.
For patients who wear removable dentures, implant-supported overdentures offer additional design choices. Locator attachments, bar-retained systems, or fixed hybrid prostheses each have distinct advantages depending on chewing needs and hygiene preferences. The restorative plan is tailored so that the prosthetic solution supports comfort, cleaning access, and a natural-looking smile.
Durability and maintenance are also part of the material conversation. High-quality ceramics and precise fabrication techniques reduce the risk of chipping or staining and contribute to long-term stability, which is why many clinicians prioritize restorative materials that combine esthetics with proven clinical performance.
Once an implant restoration is in place, ongoing care is essential to preserve both the prosthesis and the supporting tissues. Daily oral hygiene — brushing twice and cleaning between teeth with floss or interdental brushes — helps control plaque around the restoration and the implant-abutment junction. Routine professional exams and cleanings allow the dental team to monitor tissue health, detect early signs of concern, and remove deposits that are difficult to manage at home.
Regular checkups typically include assessment of the implant’s stability, evaluation of the surrounding gum tissue, and inspection of the restoration for wear or damage. Bite forces can change over time, and small adjustments may be necessary to prevent excessive stress on the implant or the prosthetic component. Early intervention can prevent minor issues from becoming more significant.
Patients with implant restorations should also be mindful of habits that place excessive force on teeth — for example, chewing very hard foods or using teeth to open packages. Nighttime bruxism (tooth grinding) can be managed with protective appliances if recommended. With sensible daily care and periodic professional oversight, implant restorations can remain functional and attractive for many years.
Implant restorations are adaptable to a wide spectrum of restorative challenges, from replacing a single anterior tooth to reconstructing an entire arch. In cases where adjacent teeth would otherwise need to be altered for a traditional bridge, implants can preserve healthy tooth structure by providing independent support for replacement crowns. This tailored approach often results in more conservative long-term outcomes.
When bone loss or medical history complicates implant placement, contemporary treatment options such as bone grafting, sinus lifts, or staged approaches enable clinicians to create a stable foundation for implants. Coordination between the surgical and restorative phases is particularly important in these cases to ensure that the final prosthesis aligns with both functional and esthetic goals.
For patients seeking a comprehensive solution, the Fishers practice brings together surgical expertise and restorative craftsmanship to streamline care under one roof. From careful planning with digital imaging to the final polish on a custom crown, each step is designed to produce a durable, natural-looking result that meets the patient’s daily needs and smile expectations.
In summary, implant restorations combine surgical stability with precise restorative design to deliver replacements that look, feel, and function like natural teeth. If you would like to learn more about how implant restorations could fit your dental needs, please contact us for additional information and to discuss potential treatment pathways.
Implant restorations are prosthetic teeth that attach to dental implants, which are titanium posts placed in the jawbone to serve as artificial tooth roots. Unlike removable dentures or tooth-supported bridges, implant restorations are anchored directly to the bone, providing greater stability for chewing and speaking. This direct support also helps preserve adjacent teeth by avoiding the need to alter healthy tooth structure for a bridge.
The final implant restoration can take the form of a single crown, a bridge, or an overdenture depending on the number of teeth being replaced. Because implants rely on osseointegration with the jawbone, the result can function and feel much like a natural tooth when planned and executed properly. Restorative design and material selection further influence how well the prosthesis blends with the surrounding dentition.
Good candidates typically have stable general health, sufficient jawbone volume, and healthy gum tissue surrounding the planned implant site. Patients with chronic medical conditions or a history of heavy smoking may require evaluation and management prior to implant therapy, while some bone deficiencies can be addressed with grafting procedures to create a suitable foundation. A thorough clinical exam and medical history review help determine individual suitability for implant restoration.
Diagnostic imaging, such as CBCT scans and digital impressions, are commonly used to assess bone quality, anatomical landmarks, and prosthetic space before proceeding. The restorative plan also considers bite relationships, aesthetic goals, and hygiene access to ensure the chosen solution meets long-term functional and cosmetic needs. Patient motivation for maintaining oral hygiene is an important factor in achieving successful outcomes.
Once the implant has integrated with the bone, the restorative phase begins with precise records such as digital scans or conventional impressions to capture the implant position and surrounding soft tissues. The dentist selects or designs an abutment and fabricates the crown, bridge, or overdenture to match the patient’s bite, color, and tooth form, often using CAD/CAM workflows to increase accuracy. Shade matching, emergence profile, and margin design are carefully evaluated to produce a natural-looking and functional restoration.
At placement, the restoration is connected to the abutment and the dentist checks occlusion, contacts, and soft-tissue contours, making fine adjustments as needed for comfort and function. Patients can expect a short series of appointments for verification and final seating, with follow-up visits to monitor healing and bite stability. At Complete Dental Care of Fishers these steps are coordinated to provide predictable esthetic and functional results.
Ceramics such as porcelain and zirconia are frequently chosen for implant crowns and bridges because they combine strength with translucency that mimics natural enamel. Metal-ceramic options may be used in situations where additional strength is required, while all-ceramic restorations are often preferred in highly visible areas for superior esthetics. Material choice takes into account factors like occlusal forces, location in the mouth, and the patient’s cosmetic expectations.
For implant-supported overdentures or hybrid prostheses, components such as titanium bars, locator attachments, or milled frameworks can be used to provide retention and support. The restorative dentist balances durability, hygiene access, and esthetic outcome when recommending specific materials and attachment systems. High-quality fabrication techniques and precise finishing are essential to reduce the risk of chipping, staining, or mechanical complications.
Daily oral hygiene around implant restorations is critical and includes thorough brushing twice a day and cleaning between teeth with floss, interdental brushes, or other recommended aids to remove plaque at the implant-abutment junction. Gentle, consistent technique helps protect soft tissues and prevent inflammation around the implant, while avoiding overly abrasive brushes and harsh chemical agents preserves restorative materials. Patients should also avoid using teeth as tools and be mindful of habits that exert excessive force on restorations.
For patients who grind their teeth, a custom nightguard can reduce stress on implant restorations and the supporting bone. Tobacco cessation is strongly encouraged because smoking impairs healing and increases the risk of implant complications. If there are changes in fit, discomfort, or signs of inflammation, contacting the dental team promptly allows early assessment and management.
Regular professional follow-up is important to monitor the health of the implant, surrounding gum tissue, and the integrity of the restoration, with frequency tailored to individual needs and risk factors. Many patients are seen for hygiene appointments and evaluations every three to six months initially, while stable cases may move to a maintenance schedule recommended by the dentist. These visits include professional cleaning, assessment of occlusion, and visual or radiographic checks for bone levels and component integrity.
During recare visits the dental team looks for early signs of soft-tissue inflammation, loosening of components, or wear on the prosthesis so that minor issues can be addressed before they progress. Periodic radiographs may be taken to assess bone support and implant stability according to clinical judgment. Maintaining consistent professional care supports the long-term success of implant restorations.
Yes. Implant restorations are versatile and can replace a single tooth, support multi-tooth bridges, or provide full-arch solutions such as fixed hybrid prostheses or implant-retained overdentures. Treatment planning considers the number and distribution of implants needed to support the intended prosthesis while achieving appropriate function and esthetics. In many cases implant-supported restorations offer a more conservative alternative to removing tooth structure for traditional bridges.
Comprehensive planning for multiple-tooth replacement often involves digital imaging, surgical guides, and coordination between surgical and restorative phases to ensure optimal implant positioning and prosthetic emergence. When bone volume is limited, staged approaches or bone augmentation procedures can establish a reliable foundation for the final restoration. The restorative design prioritizes hygiene access, comfort, and long-term stability for full-arch reconstructions.
Potential biological complications include soft-tissue inflammation (mucositis) and bone loss around the implant (peri-implantitis), both of which are often related to plaque accumulation or systemic risk factors. Mechanical complications can include screw loosening, component fracture, or wear of restorative materials, particularly when occlusal forces are excessive. Early recognition through regular checkups and attentive home care is the best way to limit the impact of these issues.
Management strategies depend on the nature of the problem and may include professional debridement, antimicrobial therapy, occlusal adjustments, repair or replacement of prosthetic components, and in some cases surgical intervention. Collaborative planning between the restorative dentist and surgeon helps address complex problems and restore function while preserving surrounding tissues. Timely intervention often prevents small problems from becoming more significant.
Implants transmit chewing forces to the jawbone in a manner similar to natural tooth roots, which helps stimulate and preserve bone over time and can reduce the progressive bone loss that follows tooth extraction. By providing independent support for replacement teeth, implant restorations also avoid placing additional stress on adjacent natural teeth that would otherwise be modified for a bridge. This conservative approach can support long-term oral health and function.
Maintaining healthy surrounding gum tissue and controlling plaque are essential for preserving both the implant and the bone that supports it. Regular monitoring and preventive care allow the dental team to detect changes in bone level or tissue health early and take corrective action. When combined with appropriate restorative design and patient adherence to hygiene recommendations, implants can be an effective tool for preserving oral structure and function.
Receiving both surgical placement and restorative treatment in a single practice improves communication and continuity of care, allowing the treatment team to coordinate implant position, prosthetic design, and timing more efficiently. This integrated approach reduces the risk of miscommunication between providers and supports a cohesive digital workflow from imaging and planning to final restoration. Patients benefit from smoother logistics and a unified plan that aligns surgical and aesthetic objectives.
Having surgical and restorative expertise under one roof also facilitates immediate troubleshooting and timely follow-up when adjustments are needed, which supports predictable outcomes and long-term maintenance. Many practices that offer in-office implant placement and CAD/CAM restoration technology can streamline appointments while maintaining clinical oversight at each step. Complete Dental Care of Fishers provides coordinated surgical and restorative services to help patients achieve reliable, natural-looking implant outcomes.
Email: