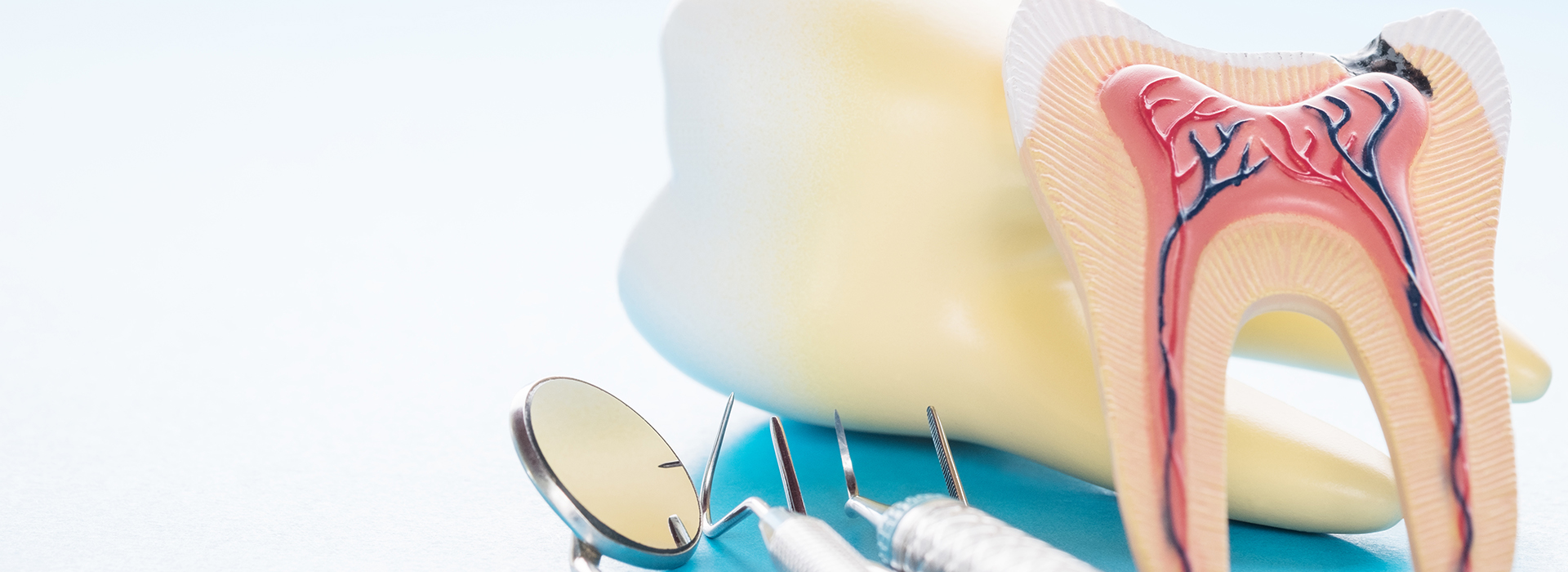
If a dentist recommends a root canal, try not to worry—this treatment is a predictable, well-established way to stop pain and preserve a natural tooth. Modern root canal therapy is performed with technologies and techniques that make the experience far more comfortable than many people expect; in many cases the procedure feels no more involved than having a large filling placed.
Our goal is simple: relieve discomfort, remove infection, and restore the tooth so you can chew and smile with confidence. At the office of Complete Dental Care of Fishers, we focus on careful diagnosis, gentle treatment, and clear communication so you understand what to expect at every step.
When the soft tissue inside a tooth (the dental pulp) becomes inflamed or infected, simply leaving the problem untreated can lead to persistent pain, spread of infection, and ultimately the loss of the tooth. Root canal therapy allows your dentist to remove the diseased tissue, clean and disinfect the inner chamber, and then seal the space to prevent reinfection — all while preserving the visible portion of the tooth.
Keeping a natural tooth has many advantages. A retained tooth helps maintain proper chewing function, supports surrounding teeth and bone, and avoids the extra procedures often needed when a tooth is missing. For many people, a successful root canal followed by a well-designed restoration lets the tooth function normally for many years.
Thanks to advances in local anesthesia, rotary instruments, and filling materials, the procedure has become both more precise and more comfortable. Your dentist will tailor the approach to the specific tooth anatomy and condition so you receive effective care with the least discomfort possible.

Teeth are not solid blocks; each contains an inner chamber that houses nerves, blood vessels, and connective tissue. When a deep cavity, crack, or blunt trauma allows bacteria to reach this tissue, inflammation and infection can follow. Because the pulp sits inside a rigid shell of enamel and dentin, pressure increases and pain can escalate quickly.
Symptoms that suggest the pulp may be compromised include lingering sensitivity to hot or cold, prolonged ache when biting, unexplained changes in tooth color, swelling around the gum, or a persistent toothache that disturbs sleep. Sometimes a tooth with an infected pulp causes minimal or no pain initially and is discovered on a routine exam or x-ray that shows changes at the root tip.
Early diagnosis is important. A thorough clinical exam combined with diagnostic imaging helps determine whether root canal therapy is the appropriate treatment or if alternative care is better suited. Prompt attention often means a simpler procedure and a more predictable result.
Not every twinge signals the need for a root canal, but certain patterns of symptoms are strong indicators that the dental pulp is involved. If you notice persistent or worsening pain, sensitivity that lingers long after a hot or cold stimulus, visible darkening of a tooth, or swelling near a tooth, schedule an evaluation without delay. A timely appointment can prevent progression and protect surrounding tissues.
Other signals include discomfort when biting, a tooth that feels loose, or recurrent gum swelling and drainage near a specific tooth. Even if symptoms seem intermittent, they can reflect an underlying infection that requires professional treatment.
Your dentist will discuss findings, review imaging, and recommend a treatment plan tailored to the tooth’s condition. When a root canal is recommended, the decision is driven by the goal of preserving the tooth and eliminating sources of pain or infection.
Pain that persists or wakes you at night often indicates significant irritation or infection within the tooth.
Sensitivity that lingers after hot or cold foods suggests the pulp is injured and unable to recover on its own.
Discoloration, chips, or cracks can expose the inner tissues and lead to infection that requires intervention.
Signs of localized swelling or drainage, and a tooth that feels mobile, are indications that infection may have reached supporting structures.
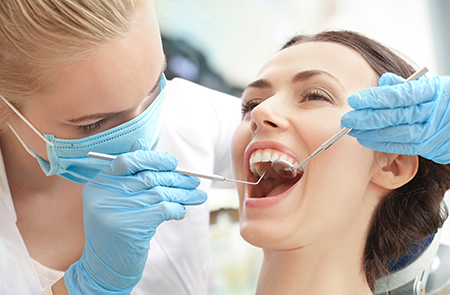
Addressing pulpal disease promptly reduces the chance that an infection will spread to adjacent bone or soft tissues. Delaying care can lead to more complex treatment needs, increased discomfort, and a higher risk that the tooth will eventually require extraction. Early intervention helps contain the problem and preserves more of the natural tooth structure.
A quick response also improves the predictability of healing. Once the infected tissue is removed and the canals are cleaned and sealed, the body is better able to repair the surrounding bone and gum tissue. Follow-up care and a proper final restoration further support long-term success.
Your dentist can explain how soon treatment should begin based on the exam and x-rays. In many cases, starting care quickly results in fewer appointments and a smoother recovery.
Root canal treatment begins with a careful examination and targeted local anesthesia so you remain comfortable throughout the procedure. The dentist creates a small access opening in the chewing surface or back of the tooth to reach the pulp chamber and the canal system within the roots.
Using specialized files and irrigating solutions, the dentist gently cleans and shapes each canal to remove inflamed tissue and bacteria. These steps are followed by thorough disinfection and placement of a biocompatible filling material to seal the canals. In many cases, a temporary filling or buildup is placed and the tooth is restored with a permanent crown at a later appointment to protect the remaining structure.
The complexity of the tooth — for example, the number and curvature of the canals — determines whether the procedure is completed in a single visit or staged over two or more sessions. For patients who feel anxious, sedation dentistry options are available to keep the experience calm and manageable.
After the canals are sealed, returning for the recommended permanent restoration is essential. A properly fitted crown or onlay restores strength and function, helping the treated tooth last for many years.
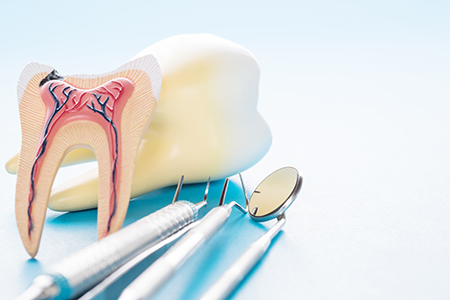
Following treatment, most patients experience relief from the acute toothache that brought them in. Mild soreness around the treated tooth and surrounding gum may be present for a few days as the tissues respond to the procedure and heal. Over-the-counter pain relievers typically manage this discomfort, and your dentist will advise on specific medications if needed.
Protecting the treated tooth until it receives a permanent restoration is important because teeth without a full crown can be more prone to fracture. During this interim period, avoid very hard or sticky foods on the treated side and follow any temporary-care instructions provided by the office.
Continue your regular oral hygiene routine—brushing gently and flossing daily—since healthy gums and clean teeth support the long-term success of the root canal-treated tooth. Attend follow-up appointments so your dentist can confirm healing and complete the final restoration when appropriate.
With proper treatment and regular care, a tooth that has undergone root canal therapy can remain functional for many years, often for the rest of a patient’s life.
At the office of Complete Dental Care of Fishers, we strive to provide clear explanations and thoughtful care before, during, and after root canal therapy. If you have concerns about a troubling tooth or would like to learn more about treatment options, please contact us for more information.
A root canal procedure is the best way to save a tooth that has been damaged by decay or injury and preserve your natural smile. The alternative is an extraction and treatment to replace the tooth. While at times a tooth is non-restorable and an extraction is the only option, when possible, it’s best to try and save your natural tooth. With proper care, a tooth with root canal therapy can serve your smile well for many years to come.
Despite lingering myths from before the age of modern dental anesthesia and technology, having a root canal procedure today is as routine and comfortable as visiting the dentist for a filling. While the procedure is performed under local anesthesia with your tooth completely numbed, we can also discuss options in dental sedation.
Whether the symptoms of a dental infection subside after a course of antibiotics, a draining abscess provides you with some temporary pain relief, or a tooth with radiographic evidence of pathology has not yet developed symptoms, it’s essential, before an infection worsens or occurs, to have a root canal procedure performed. In this way, the tooth can be disinfected, filled, and sealed to protect your health and avoid further problems.
If you have sustained a dental injury, have a toothache, jaw pain, swelling, or are experiencing any other unusual and uncomfortable oral symptoms, contact our office immediately for care. Dental problems that have not been evaluated and treated can significantly worsen, producing more severe damage and consequences for the involved teeth, your oral health, and even your overall wellbeing. Once you get in touch with our office, our friendly and compassionate office team will get you in for care at your earliest convenience.
While some root canal procedures can be completed in one visit, others may involve 2 or 3 appointments. How long it takes depends on various factors, including active infection, the number of canals in the tooth, and the tooth’s location or anatomy.
With a success rate that exceeds 95%, root canal therapy remains the most effective procedure to save a tooth in which the inner vital tissues have been damaged. However, as with all healthcare procedures, there are a small percentage of cases where the teeth become symptomatic a second time. The good news is that many of these teeth can still be saved with root canal retreatment or a minor surgical procedure known as an apicoectomy.
The best ways to maintain a tooth with root canal therapy are to get the proper restoration required to rebuild and protect the tooth, maintain proper oral hygiene, and schedule appointments for routine dental checkups and care.
Saving a tooth with root canal therapy is a wise investment that, in the long run, is typically less costly and invasive than having the tooth extracted and replaced with a fixed bridge or implant. As far as the exact cost of care, it can vary depending on which tooth is being treated. Many dental insurance plans provide coverage for root canal therapy. At the office of Complete Dental Care of Fishers, we do our best to optimize your dental benefits and minimize your out-of-pocket expenses. Our staff will answer all your questions about the cost of care and discuss all your payment options.
At the office of Complete Dental Care of Fishers, we use the latest technology and most effective methods of care to provide precise and gentle care. Our reputation for excellence is based upon a consistent record of achieving successful treatment outcomes while providing prompt, stress-free, and convenient treatment for every type of dental need.
A root canal is a dental procedure that removes diseased or damaged dental pulp from inside a tooth. The dentist cleans and fills the internal canals to eliminate infection and prevent further damage. By removing the infected tissue, the procedure relieves pain and preserves the natural tooth structure.
Modern root canal therapy is typically comfortable and can often be completed with the same patient comfort as a routine filling. When a tooth can be preserved, root canal treatment is generally preferred over extraction because it maintains chewing function and bone support. At the office of Complete Dental Care of Fishers we use advanced instruments and techniques to provide precise, gentle care.
Common signs that a tooth may need root canal therapy include persistent or severe toothache that wakes you at night. Increased sensitivity to hot or cold foods, pain when biting, and swelling around the tooth are also warning signs. A tooth that has become darkened or discolored after an injury can indicate internal damage to the pulp.
Some teeth that require root canal therapy do not produce noticeable symptoms but show problems on X-rays during a routine exam. If you notice any of the signs above, prompt evaluation is important to prevent the infection from spreading and causing more damage. Early diagnosis improves the chances of saving the tooth with conservative treatment.
A typical non-surgical root canal begins with numbing the area using local anesthesia so the procedure is painless. The dentist then creates a small access opening, removes the diseased pulp, cleans and shapes the canal system, and disinfects the interior of the tooth. Once the canals are clean, they are filled with a biocompatible material such as gutta-percha to seal the space and prevent reinfection.
Some root canals are completed in a single visit while others require two or three appointments depending on the tooth’s anatomy and the presence of infection. When needed, oral sedation or other sedation options can be used to help patients who experience anxiety or have a sensitive gag reflex. Your dentist will explain the anticipated treatment timeline and any steps required before or after the procedure.
With modern anesthesia and techniques, most patients experience little to no pain during a root canal procedure. The objective is to remove the source of pain—the infected pulp—while keeping you comfortable throughout the appointment. Dentists use local anesthetic and may offer sedation to ensure a calm, pain-free experience.
After the procedure, it is normal to have mild to moderate soreness for a few days as the surrounding tissues heal. Over-the-counter pain relievers are often sufficient to manage discomfort, and your dentist will advise you if a prescription medication is necessary. If pain worsens, swelling increases, or you develop fever-like symptoms, contact the dental office for prompt re-evaluation.
Immediately after a root canal you may experience numbness from the local anesthetic and should take care not to bite your lips or tongue until sensation returns. It is common to have some tenderness when chewing, and your dentist may adjust the bite or recommend avoiding chewing on the treated side for a short time. Following any prescribed medications and basic home-care instructions supports a smooth recovery.
Maintaining good oral hygiene and keeping scheduled follow-up visits helps ensure proper healing and long-term success of the treated tooth. If antibiotics were prescribed to control infection, it is important to finish the full course as directed by your dentist. Contact the office if you notice increased pain, persistent swelling, or any signs of continued infection.
A crown is often recommended after root canal therapy because a treated tooth can become more brittle and prone to fracture. A properly fitted crown restores strength, protects remaining tooth structure, and helps rebuild chewing function. Crowns are especially important on back teeth that endure heavy biting forces.
In many cases a temporary restoration is placed immediately and a permanent crown is scheduled once healing is confirmed and the final restoration is fabricated. Delaying placement of a protective restoration can increase the risk of fracture or recurrent problems, so timely restoration is important. Your dentist will discuss the best restorative option based on the tooth’s remaining structure and your functional needs.
When performed and restored properly, root canal therapy has a high long-term success rate and treated teeth can last many years or a lifetime. Successful outcomes depend on removing infection, sealing the canals effectively, and restoring the tooth with an appropriate final restoration. Regular dental checkups and excellent oral hygiene are key factors in preserving the treated tooth.
Several factors influence longevity, including the quality of the restoration, the tooth’s location, and your overall oral health and habits. Avoiding heavy or inappropriate forces on the tooth and addressing any new dental disease promptly will help extend its lifespan. If a treated tooth develops recurrent infection or structural issues, retreatment or further restorative care may be considered.
An alternative to root canal therapy is extraction of the affected tooth, which removes the source of infection but results in the loss of the natural tooth. After extraction, replacement options such as dental implants, bridges, or dentures can restore function and appearance but each has different clinical implications. Preserving a natural tooth with root canal therapy is often preferred when the tooth is restorable and has adequate supporting bone.
The decision between root canal therapy and extraction depends on factors such as the tooth’s restorability, bone support, overall health, and patient preference. Your dentist will review the pros and cons of each option and recommend the most conservative and predictable solution to meet your long-term oral health goals. When extraction is chosen, the dentist will discuss appropriate replacement strategies to maintain oral function and prevent drifting of adjacent teeth.
Seek emergency dental care if you experience severe uncontrolled tooth pain, rapid swelling of the face or gums, or signs that an infection is spreading. A draining abscess, trouble breathing or swallowing, or a fever accompanying dental pain are signs that require immediate evaluation. Prompt treatment reduces the risk of the infection worsening and helps preserve surrounding tissues.
Complete Dental Care of Fishers offers prompt evaluation and modern treatment options to address urgent endodontic needs and manage infection safely. Early intervention can limit damage and often allows the dentist to save the tooth with root canal therapy rather than choosing more invasive alternatives. If you suspect an emergency, contact your dental office right away to arrange timely treatment and pain control.
Yes, root canal treatment can be performed for anxious patients using local anesthesia combined with oral sedation or other sedation options when appropriate. Sedation helps patients remain relaxed and comfortable, and it is especially useful for those with dental phobia, a sensitive gag reflex, or complex treatment needs. Your dentist will review medical history and discuss sedation risks and benefits before recommending the best approach for your situation.
Pre-appointment instructions may include fasting or adjusting medications depending on the chosen sedation method, and a responsible adult may be required to accompany you home. The dental team will monitor you closely throughout the procedure to ensure safety and comfort, and they will provide post-operative instructions for recovery. Discuss any concerns about anxiety or sedation with your dentist so the treatment plan can be tailored to your needs.
Email: